 Photo: Getty Images
Photo: Getty Images
The name of the disease is a bit of a tongue-twister, especially when paired with a related condition, diverticulosis. But become familiar with the word “diverticulitis,” which can be an outcome of diverticulosis, and you just might find ways to avoid it. Better that it not be part of your daily vocabulary.
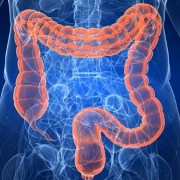
Both “d” words come into play when looking for diverticular disease. In simplest terms, diverticulosis means that the lining of the colon is protruding or herniating through the muscle wall of the colon, producing sacs or outpouches. When the small sacs, or diverticula, become infected or inflamed, that’s diverticulitis, sometimes compounded by abscesses, perforations, fistulas, and a narrowing of the colon. Diverticulitis can cause episodes of abdominal pain, or attacks, that are not pleasant.
The risk factors for diverticulitis -- including obesity, sedentary lifestyle and low-fiber diets -- are not surprising, given their connection to many other ailments. Research presented at an American Academy of Physician Assistants convention in June 2011 focused on obesity, finding a connection between diverticulitis and body mass index (BMI). In reviewing cases of 71 patients at a gastroenterology practice in New York, researchers found that fewer than one-quarter of the patients with diverticulitis had a healthy BMI. In fact, 39 percent were overweight and almost 37 percent were obese.
The Mayo Clinic noted that age is the most significant risk factor in diverticulitis, with the condition often hitting those over 40. Age brings on pressure imbalances in the colon (possibly from constipation), along with a thinning of the colon wall and an intestinal environment that’s more likely to develop diverticula.
The other major risk factor is a previous history with diverticulitis, the Mayo website said. One attack can lead to another attack down the line. Sometimes antibiotics can tame the attacks; often surgery is the answer. But the site did note that about 30 to 40 percent of people who have diverticulitis once will never develop it again.
Fiber intake comes into the discussion because fruits, vegetables and whole grains, consumed with adequate water, help move stool through the colon, thereby reducing pressure. The association between low-fiber diets and diverticulitis has not been proven, said the National Digestive Diseases Information Clearinghouse, but it is a dominant theory, with the finger pointing at modern American diets containing too much processed food.
It’s important to note that experts have not ruled out genetics as a predisposing factor in diverticulitis.
Sources:
“Recurrent Diverticulitis Often Requires Surgery.” Mayo Clinic. Web. 24 Aug. 2011.
http://www.mayoclinic.org/medical-edge-newspaper-2010/dec-17a.html
“Overweight and obesity linked to diverticulitis.” The Clinical Advisor. Web. 24 Aug. 2011.
http://www.clinicaladvisor.com/overweight-and-obesity-linked-to-diverticulitis/article/204320
“Diverticulosis and Diverticulitis.” National Digestive Diseases Information Clearinghouse. Web. 24 Aug. 2011. http://digestive.niddk.nih.gov/ddiseases/pubs/diverticulosis/index.aspx
“Risk Factors.” Diverticulitis Foundation of America. Web. 24 Aug. 2011. http://www.diverticulitisfoundation.org/risk-factors
Reviewed August 24, 2011
by Michele Blacksberg R.N.
Edited by Jody Smith





Add a CommentComments
There are no comments yet. Be the first one and get the conversation started!