At some point in your treatment for endometriosis, your doctor will likely recommend surgery. What type of surgery, how the surgery is performed and, most importantly, the reason for the surgery should all be part of your decision as to whether or not to undergo any operation.
Typically, experts agree that an integrative approach—one that uses both medical and surgical treatments—works best for managing endometriosis. As to which is better, well, no one knows. There have been no head-to-head clinical trials comparing the two.
The most commonly used surgeries for endometriosis are:
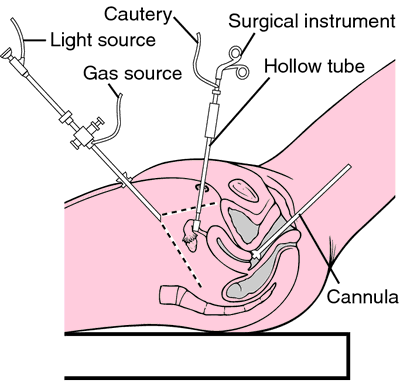
Laparoscopy. This is a minimally invasive procedure to remove the "lesions" of endometriosis. During a laparoscopy, the surgeon views your abdominal area and reproductive organs through a tiny lighted telescope inserted through one or more small incisions in your abdomen. From there, the surgeon can either cut out the endometrial tissue or destroy it with heat or laser.
Laparotomy. This is a more involved surgery requiring an abdominal incision. The major negative of this type of surgery is that it typically requires a much longer recovery time involving more pain and disability.
Studies are mixed as to which type of surgery is best. Some show lower rates of recurrence and higher rates of pregnancy with laparotomy; others show just the opposite. Both types of surgery carry a risk of scar tissue and adhesions, which could lead to infertility, make pain worse, require additional surgeries or damage other pelvic structures. Adhesions form as a result of injury or trauma to the peritoneum, the clear membrane that covers the inside of the abdomen and all abdominal and pelvic organs, except the ovaries. When healthy, this membrane is slippery. Once injured, however, the immune system kicks in to repair things, leading to inflammation and the production of sticky scar tissue called a fibrin matrix.
Normally, these bands of scar tissue dissolve through a biochemical process called fibrinolysis, the process that enables a cut on your finger and any resulting scab to heal. But surgery reduces levels of blood chemicals needed for fibrinolysis, meaning these fibrous bands may not dissolve; instead, they develop into adhesions. Adhesions may form within a couple of weeks after surgery, within months or even after a year or more.
Other, less common surgeries for endometriosis include:
Presacral neurectomy (PSN). This surgery is performed to help with menstrual pain, not to get rid of the endometrial lesions. It basically cuts the presacral nerve, which provides sensation to the uterus and pelvic floor. One study comparing PSN with laparotomy or laparoscopy found a much higher "cure" rate in those undergoing PSN, although women undergoing the more conservative surgery had no complications compared to 11 in the 60 women undergoing PSN. The complications were primarily constipation and some urinary urgency (suddenly feeling like you have to go to the bathroom). None of the women experienced any sexual dysfunction or urinary retention (when urine is left in bladder after urinating).
Laparoscopic uterosacral nerve ablation (LUNA). In this procedure, the nerves that provide feeling to the cervix and lower part of the uterus are destroyed laparoscopically.
A review of studies on PSN and LUNA found they worked best for women whose pain was not caused by endometriosis. The review also found that combining PSN with a laparoscopy relieved pain better than laparoscopy alone, although there was a higher rate of complications in women undergoing PSN. The primary adverse effects were constipation and urinary urgency.
Hysterectomy. Hysterectomy involves the removal of the uterus. Sometimes, the cervix is also removed. In a hysterectomy with bilateral oophorectomy, the ovaries are also removed. Although hysterectomy is often performed in women with endometriosis, results are mixed. If the ovaries are left and so continue to provide estrogen (which stimulates the growth of endometrial tissue), then women have a sixfold greater risk of developing recurrent pain, and an 8.1 times greater risk of having another operation than if they had their ovaries removed.
Plus, women who retain their cervix have a 10 percent risk that they will need another surgery to remove the cervix because of bleeding, pain or cervical cancer, particularly if they also have endometriosis and adhesions.
The bottom line is that although medical treatments for endometriosis can have side effects, stopping the medication typically stops the side effects. But surgery is permanent; if a surgical procedure leaves adhesions, you may have to cope with further surgeries and pain for years.
Only you and your doctor can decide which options are best for treating your endometriosis. Make sure you consider your options carefully, ask lots of questions, get a second opinion if necessary and are aware of all the potential benefits and risks of treatment.
References
Winkel CA, Scialli AR. Medical and surgical therapies for pain associated with endometriosis. J Womens Health Gend Based Med. 2001;10(2):137-162.
Frishman GN, Salak JR. Conservative surgical management of endometriosis in women with pelvic pain. J Minim Invasive Gynecol. 2006;13(6):546-558.
Jarrell J, Mohindra R, Ross S, Taenzer P, Brant R. Laparoscopy and reported pain among patients with endometriosis. J Obstet Gynaecol Can. 2005;27(5):477-485.
Swank DJ, Van Erp WF, Van Repelaer Driel OJ, Hop WC, Bonjer HJ, Jeekel H. A prospective analysis of predictive factors on the results of laparoscopic adhesiolysis in patients with chronic abdominal pain. Surg Laparosc Endosc Percutan Tech. 2003;13(2):88-94.
Gutt CN, Oniu T, Schemmer P, Mehrabi A, Buchler MW. Fewer adhesions induced by laparoscopic surgery? Surg Endosc. 2004;18(6):898-906.
Zullo F, Palomba S, Zupi E, et al. Long-term effectiveness of presacral neurectomy for the treatment of severe dysmenorrhea due to endometriosis. J Am Assoc Gynecol Laparosc. 2004;11(1):23-28.
Latthe PM, Proctor ML, Farquhar CM, Johnson N, Khan KS. Surgical interruption of pelvic nerve pathways in dysmenorrhea: a systematic review of effectiveness. Acta Obstet Gynecol Scand. 2007;86(1):4-15.
Martin DC. Hysterectomy for treatment of pain associated with endometriosis. J Minim Invasive Gynecol. 2006;13(6):566-572.
© 2008 National Women’s Health Resource Center, Inc. (NWHRC) All rights reserved. Reprinted with permission from the NWHRC. 1-877-986-9472 (toll-free). On the Web at: www.healthywomen.org.




Add a Comment7 Comments
Hello Everyone,
I have recently been reffered to a gynenecologist for 2 abnormal paps. When I recieved my results it said I had endometriosis cells. Im very nervous as I am only 20, and want to be having children soon. Can anyone tell me what I should expect in regards to surgery? fertlity? I they are ridiculous questions as everyones condition is different, but if anyone could share there full experience, I feel it would help me understand what's going on.
Thanks so much, Kate
October 9, 2012 - 1:28pmThis Comment
I'm only 16 and this is my story ... I went to the doctors complaining about pains and they said it was my appendix so he sent me to hospital and i was in for 3 days watching and examining me then they sent me home on the Wednesday and i went back in that night because i was in that much pain i was crying and they said if you bring her back in the morning we will operate on her in the afternoon so i had the operation where they removed the blood from my stomach and then they said i had Endometriousis so he booked an appointment with my doctor and told me to go to him so i did i ended up on the pill and 3 different kind of painkillers but its been 3 months later and i'm still waiting for someone to do something as im in year 11 in school i need to focas on this year completely and im not going out with friends as im too tired and in too much pain but the doctor said if these tablets i'm on don't work im have the operation where they burn the excess tissue from my stomach xx
November 4, 2012 - 4:31amThis Comment
Hi hrdg99,
Your doctor will determine the stage of endometriosis. I know mine was determined during my surgery - the doctor was able to see where it was located how much it had spread and how much damage it had caused.
Here's some additional information regarding treatments you may find useful https://www.empowher.com/condition/endometriosis/treatments?page=1.
I was able to manage the symptoms for many years before I had to have surgery, so it is manageable. But I'd encourage you to speak with your doctor to see what the best treatment option is for you.
Good luck and keep us posted on how you are doing.
Angelica
November 21, 2011 - 5:03pmThis Comment
I didn't know there are stages of endometriosis. How is this determined? If not for the pain that the patient is experiencing, can endometriosis be just ignored and kept as is inside the body, since surgery can also lead to further pain (due to adhesions) and other consequences like bleeding, etc. etc.?
November 19, 2011 - 7:38pmThis Comment
I had endometriosis (stage IV) and after several surgeries to remove the endometriosis and adhesions I finally had to have a hysterectomy with bilateral oophorectomy last year. Can endometriosis still come back after you've had a complete hysterectomy?
April 7, 2011 - 4:23pmThanks,
Angelica
This Comment
Sadly, yes it can. Stage IV endo, I have had both RSO then TAH/LSO laparotomies, and now have another cyst (endometrioma) with possible ovarian remnant. Am scheduled for removal of the cyst, the remnant, a pelvic peritonectomy, and redoing the incision at the top of the vagina. I hope this third surgery will get all of the remaining endo. I am also lucky to be able have an expert surgeon at Mayo clinic AZ (I love this place so far!) and encourage women who have been told their endometriosis is severe to see a specialist, not just your normal GYN. Also, read everything you can including medical journal articles if you are comfortable, so that you know the latest research and treatments and can make the best decisions for your health. Endo implants can be microscopic and that is why sometimes the surgeon cannot remove it all during a hysterectomy. I also understand that if your surgeon has not dealt with more complex endo cases, they are reluctant to excise the endo near the bladder, bowels, ureters, etc. In this case, a 99% job is not enough, especially if you need estrogen after surgery (likely if you are young/less than 50?). The good news is that new robotic surgery is available from specialists, so the pain and recovery time can be reduced while improving the ability of the surgeon to see smaller regions of endo that need removal. Good luck, endometriosis is truly a frustrating disease and I hope advances continue to be made to understand and treat it!
April 15, 2011 - 1:52pmThis Comment
I have had four surgeries for endometriosis and this is a frustrating condition. It is so difficult to know if each is causing more or less scar tissue. My past two surgeries (the final including a fairly aggressive peritonectomy on pelvic organs) have resulted in only a very moderate reduction of pain.
April 7, 2011 - 12:15pmI hope the medical community continues to explore this disease. There seems to be widespread lack of research and understanding about it, and I was disappointed to have that observation confirmed by the great doctors at Mayo Clinic.
This Comment