Staphylococcus aureus causes a wide variety of infections. Its growing resistance to antibiotics has raised concerns about more serious outcomes. Methicillin-resistant Staphylococcus aureus, known as MRSA, has become the most common strain in some areas. Emily A. Morrell, BA, of Harvard Medical School and Daniel M. Balkin, BA, of Yale University School of Medicine provided a review.
Staphylococcus was the bacteria in the Petri dish contaminated by mold that led Alexander Fleming to the discovery of penicillin in 1928. Penicillin was commercialized in the 1940s, and the bacteria developed resistance shortly afterward.
In 1959, the British company Beecham introduced methicillin, which is a derivative of penicillin with bulky chemical units that protect the molecule from attack by bacterial enzymes. Some strains of Staphylococcus aureus developed resistance to methicillin within a few years, but MRSA remained rare until recently.
In 1974, only 2 percent of Staphylococcus aureus (staph) infections in hospital intensive care units were methicillin resistant. By 2004, the number was 64 percent.
Antibiotics used to treat MRSA include clindamycin, tetracyclines, trimethoprim-sulfamethoxazole, linezolid, vancomycin, daptomycin, and teicoplanin. “Currently, little clinical evidence exists regarding the efficacy of alternative agents,” Morell and Balkin reported.
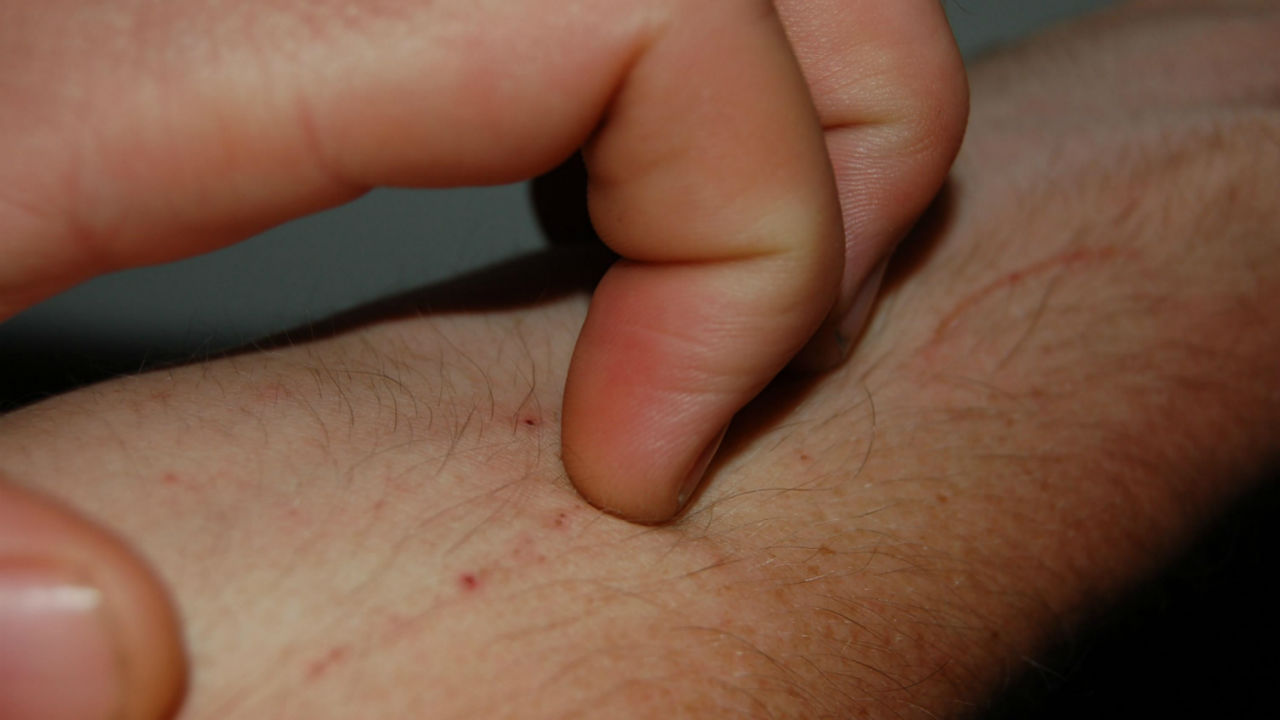
Staphylococcus aureus strains are found as harmless commensal bacteria in 30 percent of the human population. Some strains colonize the skin, and can produce infection if the skin barrier is disrupted through abrasion, burns, or other skin injury. Infection is more likely when the immune system is compromised.
Morrell And Balkin listed steroid use, genetic diseases, and HIV as examples of immunosuppressive conditions. Skin infections are the most common type of staph infections. If the bacteria penetrates deeper into the body, it can produce limb-threatening or life-threatening infections including sepsis, septic arthritis, osteomyelitis, and endocarditis.
MRSA was found only in hospital-acquired conditions until the 1990s, when the first community-acquired cases were reported in Australia and then in the United States. The spread of MRSA to the larger community implies that this strain of Staphylococcus aureus can infect healthy individuals who are not immune-compromised.
The Centers for Disease Control and Prevention (CDC) lists staph infections as healthcare-associated infections, since the majority are still acquired in hospital settings. Surgery and intravenous catheters increase the risk.
In addition, the CDC reports increased susceptibility in patients with diabetes, cancer, vascular disease, eczema, and lung disease. The CDC provides guidelines for health care professionals to prevent the prevent the spread of staph infections in healthcare settings.
References:
1. Morell EA et al, “Methicillin-resistant Staphylococcus aureus: A pervasive pathogen highlights the need for new antimicrobial development”, Yale Journal of Biology and Medicine 2010; 83: 223-233.
abstract: http://www.ncbi.nlm.nih.gov/pubmed/21165342
2. Healthcare-associated Infections. Centers for Disease Control and Prevention. Web. Oct. 4, 2011.
http://www.cdc.gov/HAI/organisms/staph.html
Linda Fugate is a scientist and writer in Austin, Texas. She has a Ph.D. in Physics and an M.S. in Macromolecular Science and Engineering. Her background includes academic and industrial research in materials science. She currently writes song lyrics and health articles.
Reviewed October 13, 2011
by Michele Blacksberg RN
Edited by Jody Smith




Add a CommentComments
There are no comments yet. Be the first one and get the conversation started!