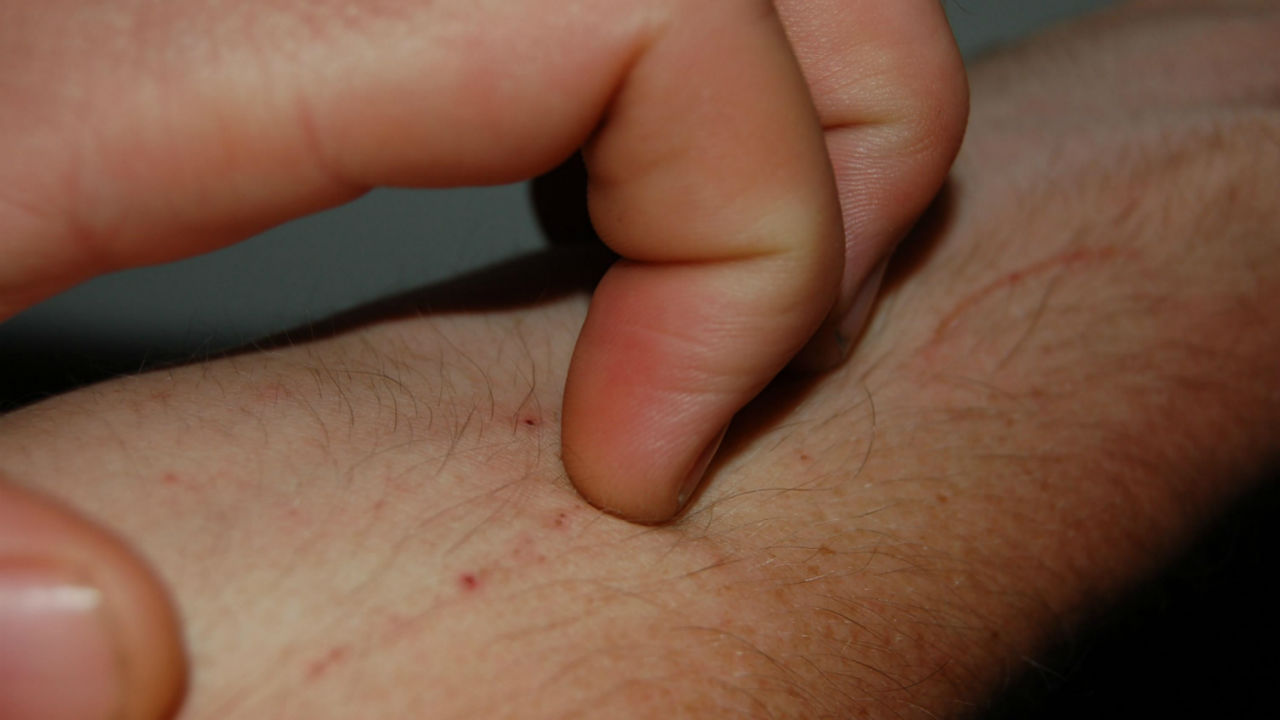
Shingles (Herpes Zoster) is caused by a reactivation of the same virus that causes chickenpox. A painful blister-like rash develops on the face, neck, chest, back or trunk that follows along the path of a nerve. The rash does goes away in two to four weeks but sometimes people are left with burning, stabbing, throbbing and/or shooting nerve pain that may continue for months or even years.
Chronic post-herpetic neuralgia (PHN) is diagnosed if the shingles pain persists after three months. People who are over the age of 50 have a 40% chance of getting PHN after a shingles out break and 75% of those over the age of 75 are at risk. The FDA has recently approved a new capsacin 8% topical patch for the treatment of PHN which can cause debilitating pain and affect one’s quality of life.
Capsaicin is made from the active ingredient in chili peppers and works as a counter irritant interfering with pain messages sent to the brain. Over the counter capsaicin cream has been available now for a number of years but the FDA approved the Quetenza patch which contains a much higher dose of capsaicin and can provide up to 12 weeks of pain reduction.
Due to the risk of side effects, the Quetenza patch must be applied during a doctor visit after a special preparation is performed on the skin. Before applying the patch, the doctor will numb the skin using topical anesthetic medication. Blood pressure is closely watched for the first couple of hours to make sure the person does not have a reaction.
The most frequently problems reported after application of the Quetenza patch are: pain, swelling, redness and itching. Other pain medication or ice packs may be used to reduce this initial pain during application. The patch will remain in place for up to 3 months. It is important to immediately wash one’s hands if the patch is ever touched and not to rub one’s eyes or other mucous membranes due to possible contact with the capsacin.
The pain of PHN can feel life consuming and can interfere with basic activities of eating and sleeping. If you or someone you know is affected by this debilitating condition, encourage them to see a doctor to determine whether a topical pain reducing patch may be of help.
If they are not good candidates for the Quetenza patch, there is also Lidocaine 5% patches that do not have side effects of blood pressure changes and are less likely to cause redness or irritation. Lidocaine 5% patches, called Lidoderm, are replaced by the patient daily rather than every three months by a doctor. Lidoderm patches have also had good success in reducing the pain of PHN.
Sources:
www.medscape.com/viewarticle/492461
www.lidoderm.com/
www.drugs.com/newdrugs/neurogesx-receives-fda-approval-qutenza-capsaicin-8-patch-postherpetic-neuralgia-phn-1772.html
Michele is an R.N. freelance writer with a special interest in woman’s healthcare and quality of care issues. Other articles by Michele can be read at http://www.helium.com/users/487540/show_articles



Add a CommentComments
There are no comments yet. Be the first one and get the conversation started!