 Michael Blann/Lifesize/Thinkstock
Michael Blann/Lifesize/Thinkstock
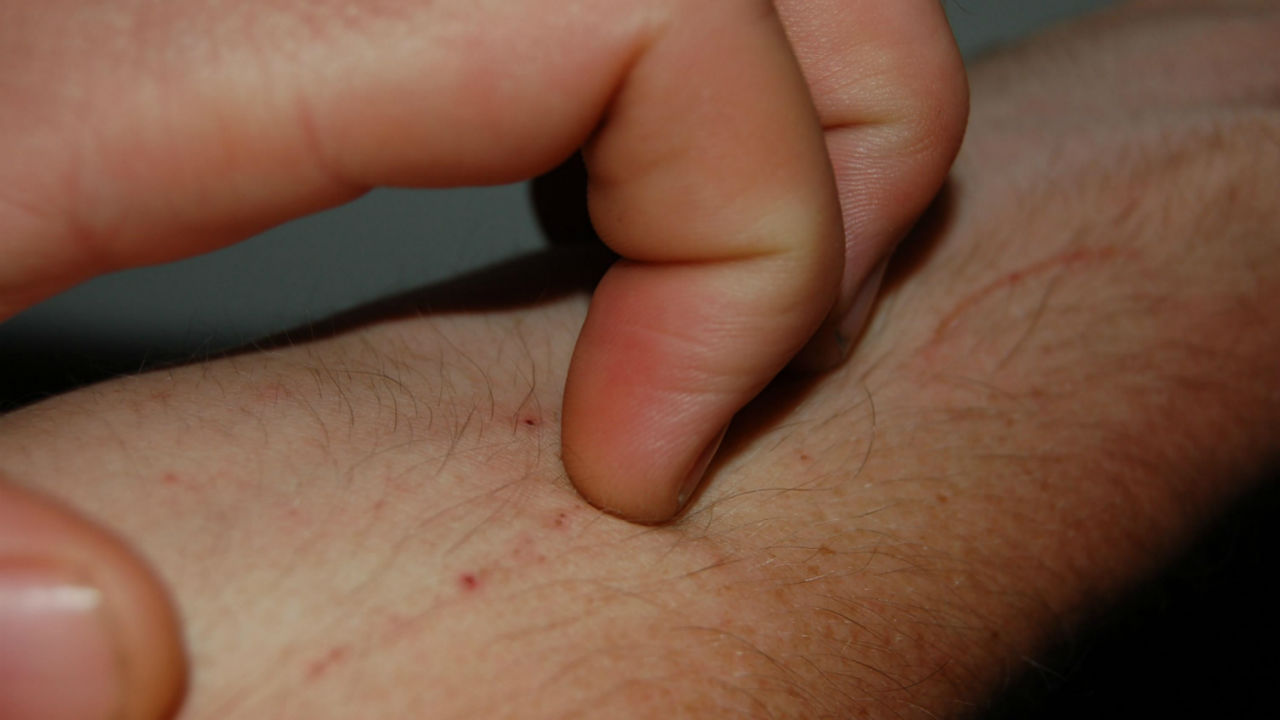
Have you have ever noticed on your skin or on someone else’s, a spattering of goosebumps that doesn’t seem to go away? Keratosis pilaris (KP) is the medical name for this benign genetic condition.
Other names for this skin disorder are gooseflesh, chicken bumps or chicken skin.
According to Medscape, keratosis pilaris affects approximately 50 to 80 percent of adolescents and 40 percent of adults. Keratosis pilaris causes numerous small, rough tan or red little bumps to form around hair follicles on the upper arms, thighs, buttocks, and cheeks.
It often occurs in those who have other dry skin conditions. KP is not curable but can be made to look less noticeable with ongoing treatments.
The exact cause of keratosis pilaris is unknown. It is thought that there is an overproduction of keratin that builds up around the hair follicles. This process is called hyperkeratinization.
Medicine.net states, “about 50%-70% of patients with KP have a known genetic predisposition and a high rate of affected family members.”
If hair becomes entrapped within the plugged follicles, the surrounding bumpy skin can become red and inflamed and be mistaken for bacterial folliculitis. When KP appears on the face, it is often mistaken for acne.
Keratosis pilaris appears worse when the skin is drier so tends to flare more in the winter and improve in the summer. Although there is no cure of KP, Mayoclinic.com says most cases tend to disappear by age 30.
Treatments and Medications:
- Exfoliants are creams that help loosen dead skin. Use of those containing alpha-hydroxy, lactic or salicylic acid or urea will exfoliate and help to soften skin.
- Steroids decrease inflammation. A doctor may prescribe a short course of topical steroid cream to reduce redness and inflammation. These creams are not used longterm due to side effects such as skin thinning.
- Retinoids can increase skin cell turnover to reduce keratin from plugging the skin around the hair follicle. Tretinoin (Retin-A Micro, Avita) and tazarotene (Tazorac) are examples of topical retinoids.
- Mild cleansers and moisturizers help to improve the skin’s texture. Gentle cleansing using Dove or if you're acne-prone, one with salicylic acid can be used once or twice a day. Lubricating lotions such as Ceptaphil or Lubriderm are often recommended to be used two or three times a day.
- Lasers can improve the appearance of KP if they are used to reduce hair growth in the areas KP occurs. Lasers used for skin resurfacing have shown limited benefit in reducing KP.
- Microdermabrasion is an in-office procedure used to exfoliate the skin. Glycolic acid peels may also be considered.
Other home practices to improve keratosis pilaris include using a loofah or Buf-Puf sponge to exfoliate the skin. Use a humidifier, especially in the winter, to increase moisture in the air and skin. And, always take time to moisturize after bathing.
Remember, on-going treatment is needed to keep keratosis pilaris under control. If you stop, it may return. However, even with treatment, KP may continue for years.
Sources:
Keratosis Pilaris (KP). MedicineNet.com.
http://www.medicinenet.com/keratosis_pilaris/article.htm
Keratosis pilaris By Mayo Clinic staff. Mayoclinic.com.
http://www.mayoclinic.com/health/keratosis-pilaris/DS00769/METHOD=print
Keratosis Pilaris. Medscape Reference.
http://emedicine.medscape.com/article/1070651-overview
Keratosis Pilaris.
http://www.formyhealth.com/keratosis%20pilaris.htm
Michele is an R.N. freelance writer with a special interest in woman’s healthcare and quality of care issues. Other articles by Michele are at www.helium.com/users/487540/show_articles/
Edited by Jody Smith



Add a CommentComments
There are no comments yet. Be the first one and get the conversation started!