 Photo: Getty Images
Photo: Getty Images
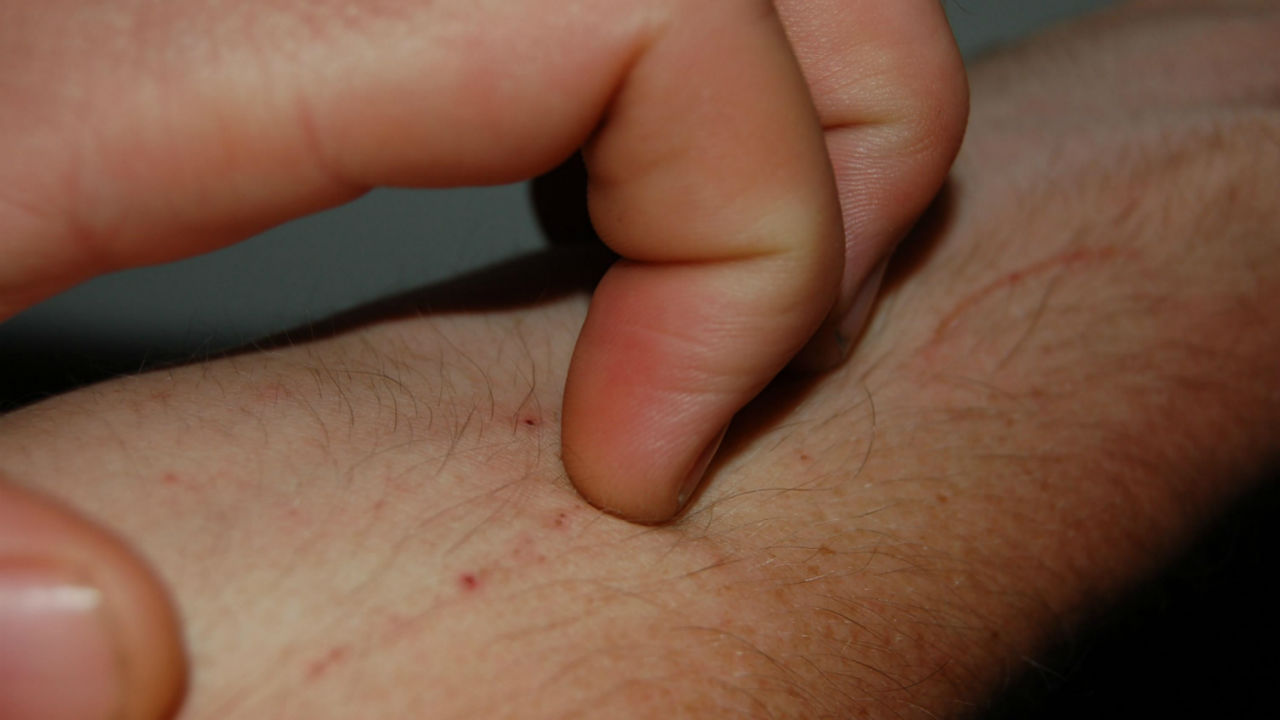
Keloids are a type of scar where the healed skin appears overly tough, thickened and irregularly shaped. Keloids may be painful or tender to touch. It is uncertain why they develop but trauma to the skin, even a minor trauma such as a bug bite, seems to be the main cause.
Medicinenet described keloids as "scars that don't know when to stop."
This abnormal healing occurs more frequently in those with brown skin such as African Americans, Latinos and Asians and in those with a family history or genetic susceptibility to them.
Keloids develop more often in those between the ages of 10-30 years old. They can occur in any person but have been found to develop between 4.5 to 16 percent in populations that are predominately Black and Hispanic.
Keloids can occur anywhere on the body but are more common on earlobes, the chest, back and arms. Sometimes a keloid can be painful, itch or become tender. This is thought to be due to abnormalities in the functioning of nerve fibers in the skin of the scar. Unfortunately, keloids may develop months or even years after the original injury to the skin.
Treatments:
- Steroid (cortisone) injections: Steroids work by decreasing the excess collagen production that make the skin overly thicken and form the keloid. These injections are mildly to moderately painful and may need to be repeated monthly for six to eight treatments. Topical steroids often cannot penetrate the keloid so are used less often.
According to Dr. Susan Taylor from brownskin.net, “one study found that 88 percent of keloids injected with triamcinalone actoneide (cortisone) decreased in size ... and itching disappeared within three to five days of injection.”
- Silicon sheets have been used with variable success in treating keloids. They must be worn for weeks to months and some doctors have found using other compression dressings to be as successful.
- Surgery to remove keloids can problematic since the rate of reoccurrence has been found to be very high -- between 45 and 100 percent. Because of this risk, it is usually recommended that surgical excision be combined with other therapies to prevent the keloid from redeveloping.
- Pressure therapy after surgery: Earlobes are a common site of keloids. Pressure earrings have been used successfully in 90 to 100 percent of patients who wore them after having surgery to remove their keloid. To see what the earrings look like go to http://www.delasco.com/pcat/3/Earrings/Pressure_Ear-P/Pressure_Ear-P/
- Radiation after surgery has been shown to have good success in preventing recurrence of a keloid. Low dose X-rays are used so the risk of developing skin cancer is low but follow-up skin checks with your doctor are recommended.
- Interferon injections after surgery act to inhibit collagen formation to decrease the likelihood of keloids reoccurring. Flu-like symptoms are a possible side effect.
- Laser removal has similar risks to surgical removal of keloids, as the chance of reoccurrence is high. Sometimes laser treatments are combined with other therapies to reduce this risk.
Prevention:
There is no specific way one can avoid developing keloids other than taking extra care to avoid skin injuries that may stimulate them to develop.
Avoid elective procedures such as ear piercings or tattoos and alert a doctor prior to any surgical procedure of your tendency to develop this type of scarring.
Sources:
Keloids. Medicine.net. Web 12, Feb. 2012.
http://www.medicinenet.com/keloid/article.htm
Scars (Keloids). Dr. Susan Taylor’s Brownskin.net. Web 12, Feb. 2012.
http://brownskin.net/scars.html
Michele is an R.N. freelance writer with a special interest in woman’s healthcare and quality of care issues. Other articles by Michele are at www.helium.com/users/487540/show_articles
Edited by Jody Smith



Add a Comment1 Comments
Kelo-cote is a 100% silicone gel for scars, which dries clear and forms a waterproof layer over the scar site. It has more clinical evidence than any other scar treatment product, with over 2,000 patients in published clinical studies. Kelo-cote may be a great non-invasive option to try, for those with keloid scarring.
February 21, 2012 - 8:46amThis Comment