 Photo: Getty Images
Photo: Getty Images
The medical literature for 2010 reported several advances in thyroid cancer research:
Thyrotropin suppression therapy may not be necessary. When the thyroid is completely removed, it is necessary for the patient to take pills to replace the the thyroid hormones. Often these are given at a high enough dose to suppress production of TSH (also called thyrotropin), the thyroid stimulating hormone. TSH is produced by the body to signal the thyroid to produce more hormones, so in a standard blood test, high levels of TSH mean the thyroid hormones are too low, and vice versa. TSH has also been associated with increased tumor growth in the most common types of thyroid cancer. Thus, it is standard to give thyroid cancer patients a high dose of thyroid hormones, in a balancing act to keep the TSH levels as low as possible without producing clinical hyperthyroidism. A randomized controlled trial reported in October 2010 reported that this therapy does not significantly increase disease-free survival time.
Hashimoto's thyroiditis is associated with thyroid cancer. The authors recommend close observation of patients with Hashimoto's disease for the development of thyroid cancer.
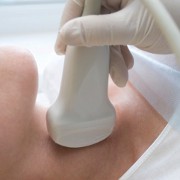
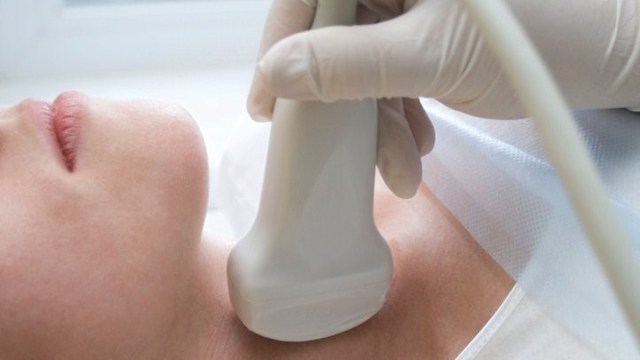
Ultrasound is effective for diagnosing medullary thyroid carcinoma. The medullary type requires different treatment, since it develops in cells that provide support functions for the thyroid, as opposed to papillary and follicular carcinomas that develop in cells that produce thyroid hormones. Surgical treatment is similar for all types of thyroid cancer, but radioiodine therapy and thyrotropin suppression therapy have no effect on the medullary type.
Surgery improves the prognosis for anaplastic thyroid carcinoma. This type of thyroid cancer is rare but deadly. Surgery, chemotherapy, and external beam radiotherapy are treatment options. A recent study shows that surgery can increase survival time, with one patient reported free of disease 80 months after surgery.
References:
1. Sugitani I et al, “Does postoperative thyrotropin suppression therapy truly decrease recurrence in papillary thyroid carcinoma? A randomized controlled trial”, J Clin Endocrinol Metab. 2010 Oct; 95(10): 4576-83.
2. Deasy J et al, “The role of thyrotropin suppression in patients with differentiated thyroid carcinoma”, Ir Med J. 2010 Jul-Aug; 103(7): 202-5.
3. Gul K et al, “The association between thyroid carcinoma and Hashimoto's thyroiditis: the ultrasonographic and histopathologic characteristics of malignant nodules”, Thyroid. 2010 Aug; 20(8): 873-8.
4. Lee S et al, “Medullary thyroid carcinoma: comparison with papillary thyroid carcinoma and application of current sonographic criteria”, AJR Am J Roentgenol. 2010 Apr; 194(4): 1090-4.
5. Palestini N et al, “Surgical treatment of anaplastic thyroid carcinoma. Our experience.” G Chir. 2010 Jun-Jul; 31(6-7): 282-5.
Linda Fugate is a scientist and writer in Austin, Texas. She has a Ph.D. in Physics and an M.S. in Macromolecular Science and Engineering. Her background includes academic and industrial research in materials science. She currently writes song lyrics and health articles.




Add a CommentComments
There are no comments yet. Be the first one and get the conversation started!