 Nelson Marques/PhotoSpin
Nelson Marques/PhotoSpin
Invasive ductal carcinoma (IDC) is the most common type of breast cancer and accounts for 80 percent of all breast cancer cases in women and 90 percent in men. Men have milk ducts too, but they are less developed than women’s ducts.
Invasive ductal carcinoma is more common after the age of 55.
IDC is the next stage on from ductal carcinoma in situ. It means that cancer has spread from the milk ducts and is now in the surrounding breast tissue.
Symptoms
Symptoms of IDC are:
• Swollen breasts or swelling in one part of the breast
• Breast pain and/or irritation
• Nipple pain
• Inward turning nipples
• Redness and scaliness of the nipple or breast skin
• Lumps under the arms
• Discharge from the nipples
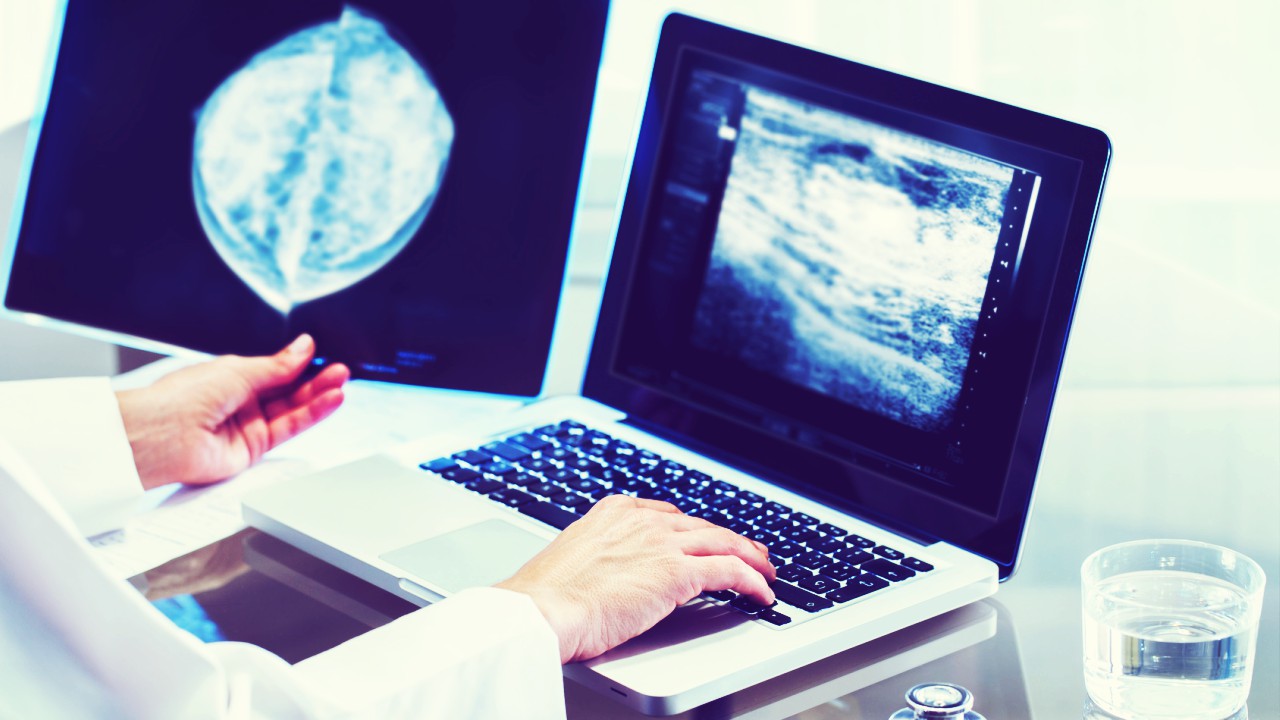
IDC is usually found on a mammogram but can also be detected via MRI scan and ultrasound. MRI uses magnetic waves and radio waves to build up a picture on the computer and ultrasound uses sound waves.
If any of your imaging diagnostic tests show something abnormal you will be offered a biopsy. This is when a sample of breast tissue is removed so that a pathologist can look at it under a microscope to see if it is cancerous.
You don’t necessarily have to have surgery in order for the doctor to get a tissue sample. There are less invasive techniques for obtaining tissue, such as:
Fine Needle Aspiration
This is when a tiny and very fine needle is inserted into the breast and cells are removed for examination.
Core Needle Biopsy
A small cut is made in the breast and a larger needle is inserted to remove cylinder-shaped samples of tissue. This type of biopsy leaves a small scar that is usually not visible after a few weeks of healing.
If the doctor cannot get a sample from either of these methods or if the test results aren’t certain, you will be offered a surgical biopsy.
Treatment
The main treatment for IDC is surgery to remove the cancer and to see if it has spread to other areas. This is called a lumpectomy. In some cases a partial mastectomy may be done (partial removal of the breast) or total mastectomy (total removal of the breast).
If you have decided on a mastectomy, you can have breast reconstruction and you may be able to have this done at the same time as your cancer surgery if you want it.
Breast cancer feeds off estrogen so reducing it or stopping it from signalling to the tumors to grow, can help prevent a recurrence of breast cancer.
Radiotherapy may then be given to try to prevent the tumors from growing back. This can be given as a beam of radiation directed at the breast or the area where the mastectomy was done.
Another method of radiotherapy is when radioactive pellets are placed where the tumor developed. This is called internal partial breast irradiation.
Other treatment methods available are chemotherapy and hormonal therapies.
Sometimes the cancer cells produce too much of a protein called HER2 and this excess HER2 signals to the breast to start growing too many cells and too quickly.
To counter this there is a drug called Herceptin that block receptors on the cells surface so that they don’t receive these growth signals. Herceptin is given via an IV.
Herceptin does have side effects and can damage your heart so it cannot be given to anyone with a heart condition or increased risk of heart disease.
If you are having chemotherapy that affects the heart you also cannot have this medication.
Follow Up
If you have been cleared of cancer you will need a check-up and physical examination every six months for the first five years and then annually after that. Regular imaging of the breasts will also be recommended.
If you are taking tamoxifen and you haven’t had a hysterectomy, you will need to see a gynecologist every year because this drug can cause uterine cancer. If you have any unusual symptoms such as bleeding in between periods, you should tell your gynecologist.
Sources:
IDC - Invasive Ductal Carcinoma, Breast Cancer Org. Web. 22 September 2012.
http://www.breastcancer.org/symptoms/types/idc
Follow-up Care for IDC, Breast Cancer Org. Web. 22 September 2012.
http://www.breastcancer.org/symptoms/types/idc/follow_up.jsp
Ductal Carcinoma (Invasive and In Situ), WebMD. Web. 22 September 2012.
http://www.webmd.com/breast-cancer/ductal-carcinoma-invasive-in-situ?page=2
What is breast cancer in men? American Cancer Society. Web. 22 September 2012.
http://www.cancer.org/Cancer/BreastCancerinMen/DetailedGuide/breast-cancer-in-men-what-is-breast-cancer-in-men
Joanna is a freelance health writer for The Mother magazine and Suite 101 with a column on infertility, http://infertility.suite101.com/ She has an A grade diploma in Neuro-psychological Immunology, which is the study of how the mind affects the immune system.
Reviewed September 24, 2012
by Michele Blacksberg RN
Edited by Jody Smith





Add a CommentComments
There are no comments yet. Be the first one and get the conversation started!