By:Sandy Powers/DivineCaroline
In 2005, I had my yearly wellness check-up with my gynecologist.
“Breast exam fine,” he said. “If your Pap test is normal, I’ll send a card. Otherwise, I’ll call. And here’s your order for a mammogram.”
A scene repeated throughout the years but this time it was going to be different.
My Pap test came back negative. One down and one to go, I thought as I made my mammogram appointment. A few days after my mammogram, the radiologist called.
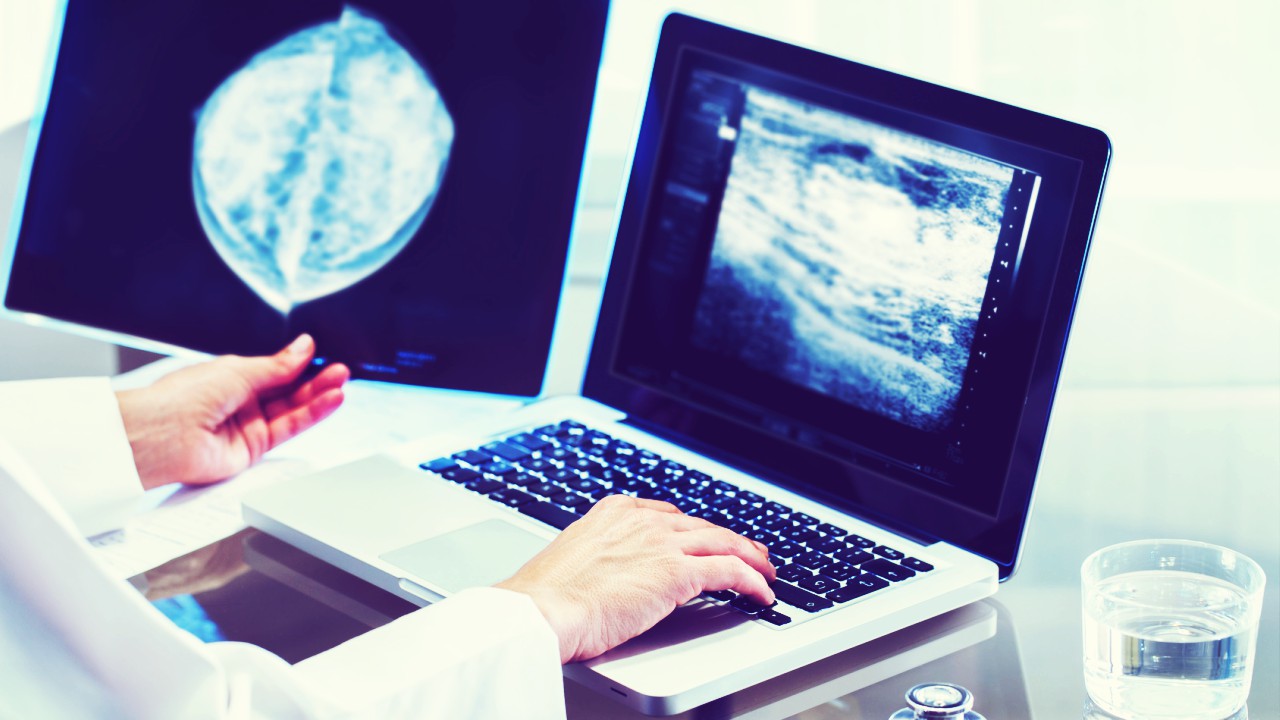
“I’d like you to have an ultrasound,” she said.
“An ultrasound? What for?” I asked.
“I think I see something. It may be nothing, but I want to make sure,” she explained.
The next day I went in for an ultrasound. A few hours later she called. “The ultrasound didn’t show anything, but I would feel better if you had a diagnostic mammogram—just to be sure,” she repeated.
“Sure,” I agreed, reassured by the ultrasound. It probably was nothing. But I was wrong. The diagnostic mammogram showed a tumor in the back of the breast close to the chest wall. The biopsy confirmed it was cancer. My best option was a mastectomy.
I am a breast cancer survivor of three years. I’m one of the lucky ones. I had a radiologist “who wanted to be sure.” Many women do monthly breast exams and have a yearly screening mammogram and as long as the doctor doesn’t call for more, they believe they are free and clear. Not so. My cancerous tumor could not be felt, even by the surgeon who performed the biopsy and knew exactly where it was. My screening mammogram never really showed anything. If I hadn’t had a radiologist “who wanted to be sure,” I probably wouldn’t be writing this article today.
Over 20 percent of breast cancers are missed because of the poor quality of the screening mammograms and the inaccuracy of the radiologists who are reading the film. A publication of the New England Journal of Medicine reported that women with dense breasts, or who had a last menstrual period within twelve months of their mammogram or who are younger than age fifty may benefit from having a digital rather than a film (or regular screening) mammogram. “This digital mammography study demonstrates how new technologies are expanding our ability to detect breast cancer earlier in more women,” continued the report. (Don’t lock yourself in the “under 50” part. Older women can also benefit.)
Digital mammograms are not as available as screening mammograms are. In fact, only about 35 per cent of U.S. mammography units are digital, the other 65 percent are conventional, or screening. Call your local hospital to find a breast-imaging center. Check the yellow pages under “mammograms” to see who offers digital mammograms. If it doesn’t say digital, it’s not digital.
Your life is worth the extra effort. More than 41,000 women will die in the United States from breast cancer this year. Don’t be one of them.
DivineCaroline.com, (Link to: http://www.divinecaroline.com/?CMP=GP_EMP_E42) is a website where empowered women like you can read and contribute stories, reviews, and forums.
Please visit our vibrant community soon.For more information visit: www.divinecaroline.com
To share your workout strategy with EmpowHer, go to www.EmpowHer.com/share