Melanoma is a form of skin cancer that begins in the melanocytes, the cells that produce melanin and give our skin its color. Typically, melanoma cancer cells are brown or black but sometimes they can appear pink, tan or even white. Malignant melanoma is another name for melanoma but both mean the same thing: melanoma cells or tumors are all malignant. (1)
Two other common skin cancers are basal cell and squamous cell cancer, which occur more often than melanoma but melanoma is far more dangerous so early detection and treatment is imperative. According to the Cleveland Clinic, of the one million cancers that will be diagnosed this year, “About 80% … will be basal cell carcinoma, 16% will be squamous cell carcinoma, and 4% will be melanoma.”
Symptoms of Melanoma:
The first skin lesions to check and monitor are moles. Moles may be flat or oval and typically are tan, brown or black. Most moles are harmless and remain small, about the size of a pencil eraser. The key is to watch for changes in color and size indicating the development of malignant melanoma.
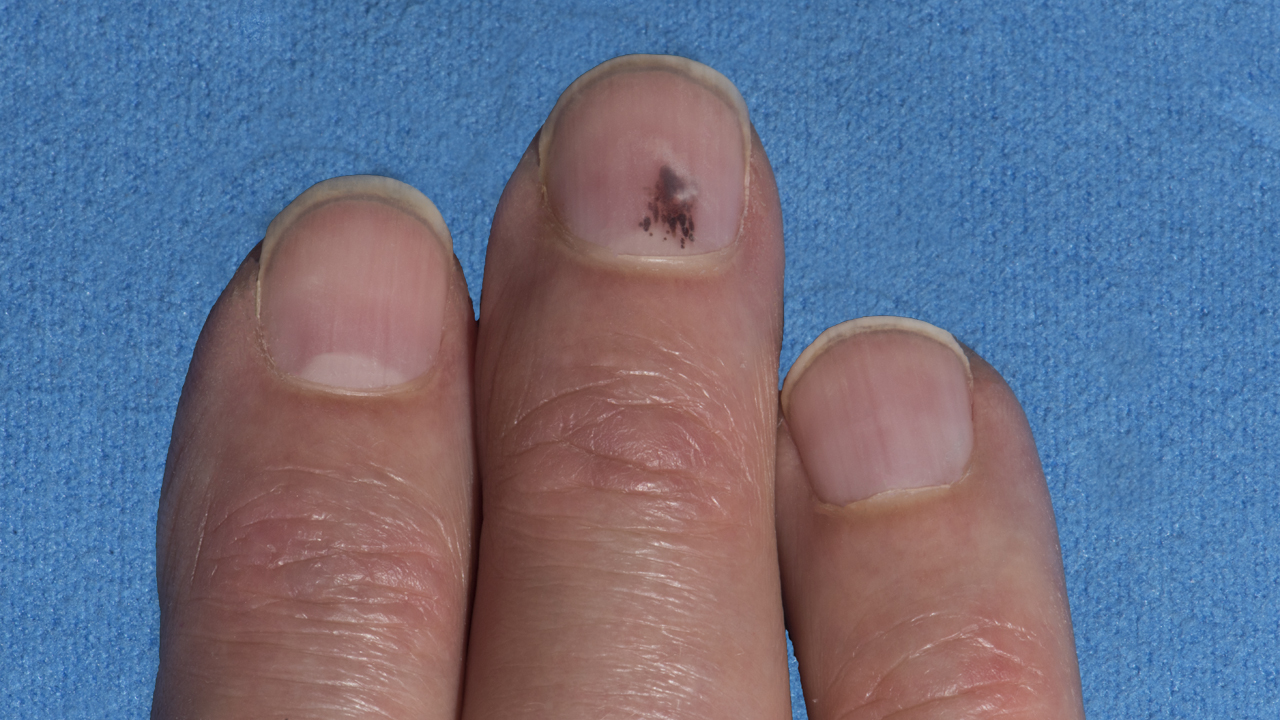
Other skin lesions that may indicate a risk of melanoma are new ones that appear on the skin or ones that change in appearance, which your doctor should check.
The common rule for checking suspicious skin spots is ABCD:
A is for asymmetry where one side of a mole or lesion appears different than the other.
B is for a change in the border so that it appears ragged or blurred.
C is for color that changes or is not uniform all over
D is for diameter that appears larger than one fourth of an inch.
There are a number of subtypes of melanoma. The two most common are superficial spreading melanoma (SSM) and nodular melanoma. About 70 percent of melanoma cases are SSM and it is the most common type of cutaneous melanoma occurring in light-skinned people. It starts as a deeply pigmented macule or plaque that develops into a cancerous lesion. Nodular melanoma occurs in 15 percent of all melanomas and starts as a uniform nodule. “Rapid growth is also a hallmark of nodular melanoma” (4)
Staging for melanoma is the process of determining how widespread the cancer has become. Melanoma is staged in two methods: clinical staging and pathologic staging. Clinical staging is based on physical exam, results of a biopsy and other imaging tests. Pathologic staging combines clinical staging results with those of biopsies of lymph nodes or any organs. (2)
Staging for melanoma is expressed using the same classification as other cancers with the TNM system. T stands for tumor, N is for lymph nodes and M is for metastasis. Numbers and letters are additionally assigned depending on the extent of the melanoma.
For example, melanoma in situ is classified as Tis, meaning that the melanoma has not spread outside the epidermis (the outer layer of skin), N0 means no spread to nearby lymph nodes and M0 means no metastasis to another area.
Treatment for malignant melanoma is determined after staging and may include: chemotherapy, surgery, immunotherapy and/or radiation therapy. Early stage melanoma may be able to be treated with surgery alone but more advanced melanoma such as metastatic melanoma may need additional treatments to attempt to eradicate the cancer. (2)
Prognosis for melanoma depends on the size and depth of the melanoma and whether it has spread to the lymph nodes. Melanoma in situ has a 100 percent survival at 5 years and 10 years while melanoma lesions greater than 4 mm have a 45 to 67 percent at 5 years and 32 to 54 percent at 10 years. (4)
Prevention is the primary method to reduce the incidence of melanoma. Regular screening assists in the early discover of melanoma lesions that need treatment. Keep wearing sunscreen even in the winter, self-inspect your skin monthly for new or changing lesions and go see a dermatologist if anything suspicious appears.
Sources:
1. What is melanoma? American Cancer Society. Web. 29, Oct. 2011.
http://www.cancer.org/Cancer/SkinCancer-Melanoma/DetailedGuide/melanoma-skin-cancer-what-is-melanoma
2. EARLY DETECTION, DIAGNOSIS, AND STAGING TOPICS. Web. 29, Oct. 2011.
http://www.cancer.org/Cancer/SkinCancer-Melanoma/DetailedGuide/melanoma-skin-cancer-detection
3. What are the survival rates for melanoma by stage? Web. 29, Oct. 2011.
http://www.cancer.org/Cancer/SkinCancer-Melanoma/DetailedGuide/melanoma-skin-cancer-survival-rates
4. Melanoma by Rebecca Tung and Alison Vidimos. Cleveland Clinic. Web. 29, Oct. 2011. http://www.clevelandclinicmeded.com/medicalpubs/diseasemanagement/dermatology/cutaneous-malignant-melanoma
Michele is an R.N. freelance writer with a special interest in woman’s healthcare and quality of care issues. Other articles by Michele are at www.helium.com/users/487540/show_articles
Edited by Malu Banuelos



Add a CommentComments
There are no comments yet. Be the first one and get the conversation started!