 Courtesy of Christina Boland
Courtesy of Christina Boland
I collect allergies like Magic Mike collects panties.
I’m allergic to everything from makeup and moisturizers to nail polishes, and yes, I’m totally going there, personal lubricants. Each of these products—even organic, hypoallergenic ones—are comprised of chemicals that cause my skin to erupt into an itchy hell.
I’m not talking about a mosquito bite itch. I’m talking about a chicken pox itch covered with poison ivy sprinkled with fire ants on top of a Jurassic-sized mosquito bite kind of itch. I lived that itch 24/7 for ten years. Yes, TEN.
I challenged my doctors to think beyond idiopathic. Some did, others were content to drug me up and call me cured.
However, I refused to quit. It took eight misdiagnoses and 19 doctors on three continents to get me to the one doctor—Dr. James A. Yiannias, Board Certified Dermatologist and Associate Professor of Dermatology at the Mayo Clinic College of Medicine in Scottsdale, Ariz.—who nailed it. I have allergic contact and atopic dermatitis: I’m allergic to chemicals and botanicals that comprise fragrances.
Diagnosing chemical allergies is tricky. It becomes exponentially harder if, like me, you have person-to-person transfer reactions. Early on, I didn’t know any of this, and neither did my doctors; they tested for every malady under the sun, everything except for chemical allergies.
Into the Itch: Years 1 & 2
My symptoms developed in early adulthood. After moving from Ohio to south Florida, I developed red, itchy, painful lumps under my left armpit. The dermatologist I saw said I had developed a sensitivity to my deodorant. His advice: Buy different deodorant. I did. None helped, some made it worse.
When the painful itchiness spread to my right armpit I also noticed a come-and-go rash-like splotch on my décolletage. The diagnosis? My skin was adjusting to its new environment and would correct itself. In the meantime, try hypoallergenic deodorant. Really? Like I hadn’t thought of that. They were all at the bottom of my waste basket.
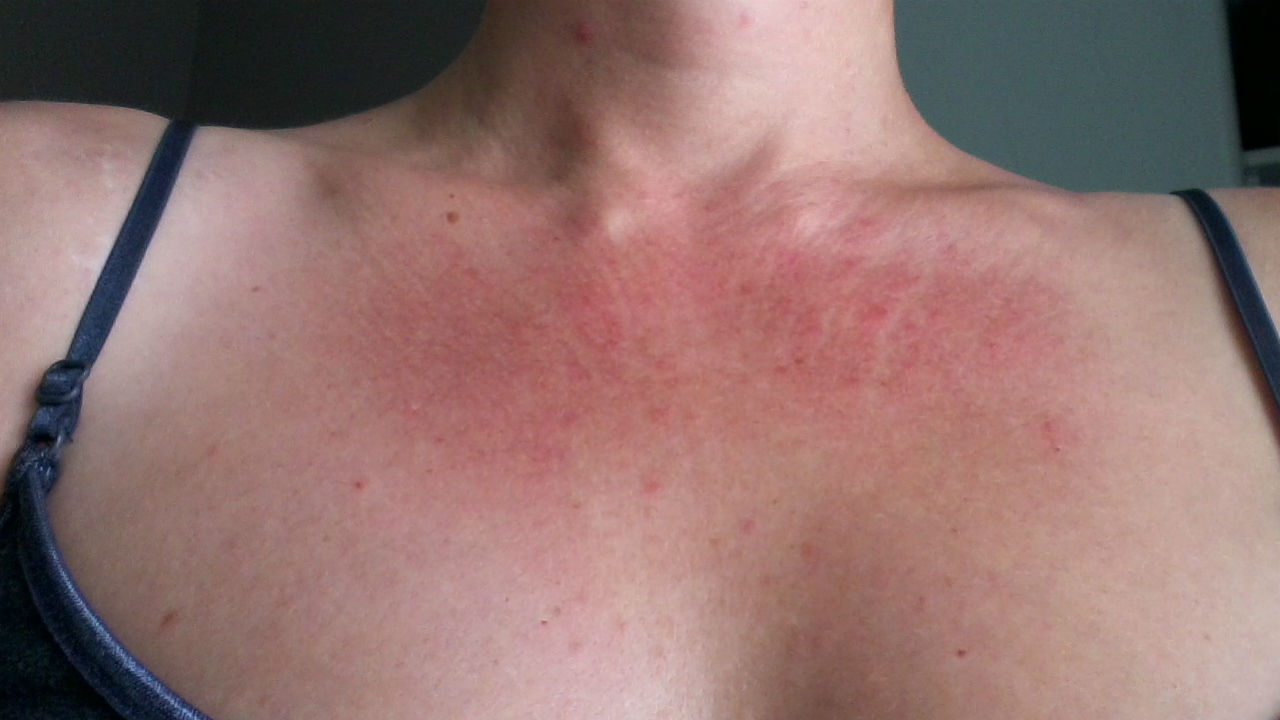
Allergic reaction on my décolletage.
Months later when it didn’t clear up, the dart throwing game began.
Armpits: Dart on hydrocortisone. This’ll clear it up.
It didn’t.
Décolletage: Dart on sunblock. Use a higher SPF.
Nope.
Don’t shave under your arms.
Seriously? Bite me.
Tea & Humors: Years 3 & 4
Itchy pits didn’t halt life. Newly married and now living in Chicago, we were about to move overseas for one year. That year turned into eight years, three continents, four countries, and 12 more doctors—all who never trusted the previous doctor’s assessment, all rerunning the same tests.
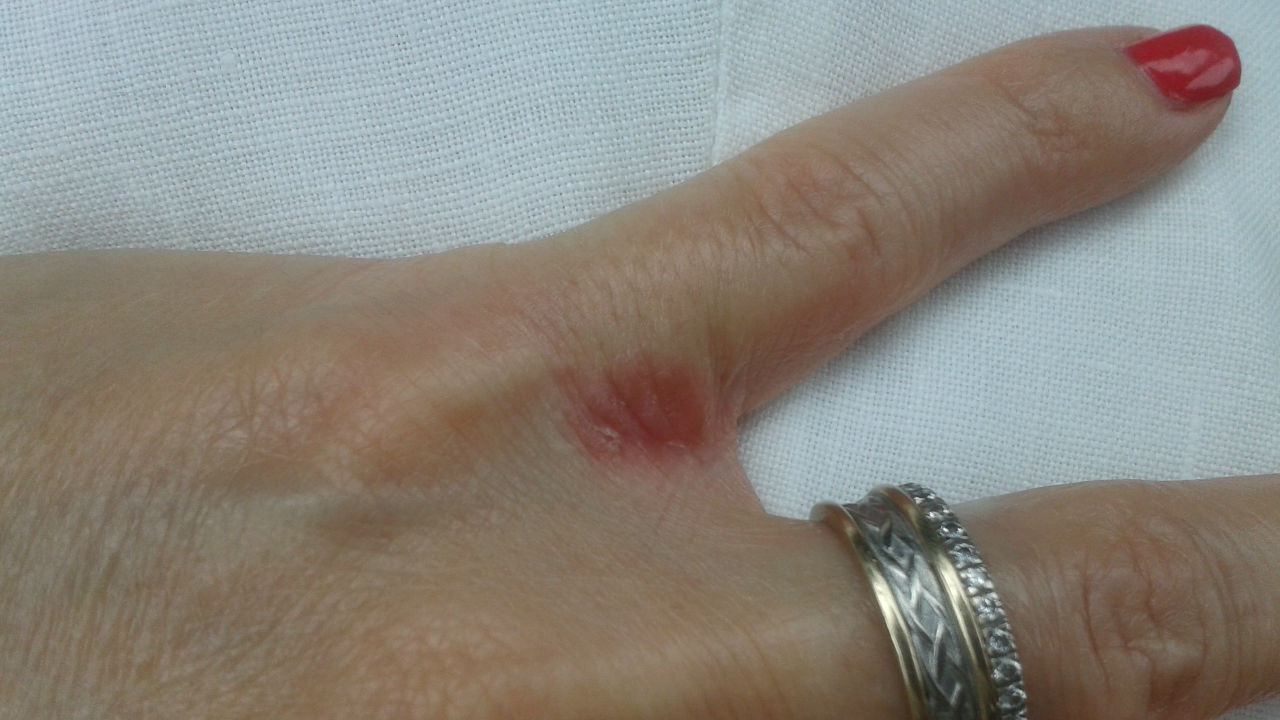
Hand dermatitis.
One German dermatologist said, “What you have izz a spezial kind of rosacea.” No other explanation. Excellent! Rosacea of the Special Kind.
His advice was to purchase black loose leaf tea, brew a batch, discard the liquid, cool the leaves, and wrap them in a cheesecloth, then put it on my face/décolletage, 20 minutes, twice a day. The tannic acid in the tea, he promised (though I can’t verify), would help heal my skin and alleviate the redness that was spreading from my décolletage north. To. My. Face.
I bought some Black Oolong, went home and followed the directions. A week later, nothing had changed. In hindsight, maybe it would have worked if what I had really was rosacea, but it was not.
Next specialist, please!
Dart on thyroid. Clear.
Dart on more blood work. All within normal ranges.
Dart on food allergies. You have a slight allergy to mussels and barley. Super.
It’s an idiopathic itch. All we can do is treat the symptoms. But nothing I’ve tried has treated the symptoms!
Dart on a hippy-sounding sensitivity to UV light. It’s polymorphic light eruption. Really? How does the sun reach my armpits in this sunshine-challenged European land?
NEXT.
Dart on adrenal glands. You’ve got low adrenal function. Fantastic. How does this tie in to being itchy? We’re not 100 percent sure. But let’s focus there right now.
Dart on steroids. Prednisone will zap it dead. It didn’t. Moreover, when I finished the month-long course, my itching rebounded and I broke out 50 times worse. That sometimes happens. Thanks for the heads-up, Doc, the rebound totally ruined my vacation.
Dart on more blood work. You’ve got a positive ANA (antinuclear antibody), but no other obvious signs of an autoimmune disorder. The itching will clear up on its own . . . eventually.
Those early days were like the Dark Ages. Honestly, I wouldn’t have been surprised to hear the next specialist tell me that the Ancient Greeks were back in town and that one of my four Humors was out of joint. With every passing day the itch grew worse.
Sleeping with Icepacks: Year 5
I looked like a Rorschach inkblot with full-fledged hives bilaterally dotting my neck, torso, armpits, and hairline. My eyelids swelled and burned. The circles under my eyes grew darker. The area around my mouth was rough and scaly. My scalp was on fire. My face was constantly workout red. To dull the itch, I slept covered with ice packs. But I looked fine, a bit tired, and with some powder, a dash of mascara, and some soft, loose fitting clothes, I didn’t look itchy.
Idiopathic was growing old and my faith in the medical community was waning.
They wanted to drug my itchiness away. I wanted to know the root cause. I wanted a name. I kept notes. I charted my itchiness. I took photographs. I looked for patterns. I organized an Itchy File: skin tests, photographs, lab results, diagnoses, medications on, tried, and failed, and authorizations. I was staging for battle for it had now taken over my life.

My Itchy File.
The Metamorphosis: Years 6 & 7
My big splotchy hives morphed into pimple-like papules. One red spot a quarter the size of a pomegranate seed had a 3-D itch radius of a grapefruit. Cluster 40 of those suckers together and I wanted to scratch the flesh from my body. I was never without an itchy patch somewhere on my body, most of the time I had multiple clusters.
I could now distinguish between a “regular” itch and one that would last for weeks.
Also, I had discerned a pattern. Seven to 10 days prior to my period, my itchiness would ramp up; during my cycle it would hold steady; the week following it abated; then the ramp-up would begin again. Doc, this has to mean something, right? Hormones sometimes do that. They can make symptoms—lupus, MS, itching—worse. That’s it!? Someone should test you for Autoimmune Progesterone Dermatitis. Can’t you?! It’s not in my lane; I’m sure you’ll find someone.
I fantasized about how to bottle a one-month dose and give it to my doctors. I guarantee after two weeks, they’d scour the planet seeking the root cause.
Invasion of My Girly Parts: Year 8
I came unglued when The Itch invaded my girly parts.
My.
Girly.
Parts.
I flew back to the States to see an allergy specialist in Florida. He diagnosed me with atopic dermatitis (eczema) and recommended that I take three showers a day and moisturize like I was trying to rehydrate a mummy. I did, and my symptoms EXPLODED. I’m putting in a referral for chemical patch testing.
BULLSEYE!!!
I flew home to the Netherlands and had my first chemical patch test—the European Standard Series. It was confirmed that I was allergic to six ingredients. My nemeses had names like phenoxyethanol and cocamidopropyl betaine.
I didn’t care that my doctor’s medical counsel, literally, was to “stay away” from the ingredients.
At home I cross-referenced my products with the test’s results. I was shocked: Nearly every single product in my hypoallergenic arsenal was a culprit. Eliminate, toss and replace. Easy-peasy, right? Only if you are fine with being a smelly, unwashed, greasy-haired, non-makeup wearing, unmoisturized slab of human flesh. I am not that person.
Moreover, I realized that those six chemical allergens had nearly 44 separate names. I was at a loss. I “washed” my hair with a smoothie of lemons and cucumbers (it totally works). I changed detergents, gave up fabric softener, and tried botanical products. Nothing changed. Then we moved home to the States.
Female Hysteria: Year 9
Nine months into reacclimatizing to American life I broke out worse than ever. I lost eight pounds in a month. I couldn’t eat or sleep. I waited for my newest allergy referral, then made my appointment, brought my Itchy File, and walked into the office of a dermatologist kind enough to tell me that what I had was not in his dermatologic repertoire.
His parting gift? A medical book - Contact Dermatitis, by Alexander A. Fisher, M.D., Third Edition. Here is where I learned more about allergen cross-reactors (what I began to call “siblings” and “cousins”), such as, If you’re allergic to Basalm of Peru, you may also be allergic to clove.
My knowledge of all things itchy was growing, but my patience was gone.
The next specialist was a misogynistic, crotchety creature who scoffed at my Itchy File, my symptoms, and then had the stones to tell me it was “female hysteria.” I ran out of swear words, then stormed out. I’m not a crier, but I bawled. This was NOT in my head. It was all over my body. I was angry, depressed, frustrated, totally pissed off, and so, SO itchy.
Next! Rheumatologist. Nothing new. Specialized gynecologist. We’re putting you on Lupron to stop your periods in hopes it will lessen your itch symptoms. Dermatology. Biopsy. New allergist. Idiopathic itch.
I was referred to an allergist three hours away. New blood work. And a new chemical allergy patch test—the North American Standard Series. I had no idea different tests existed, and that the EU and U.S. tests target slightly different allergens. For years I had been using a mix of American and European body and beauty products. Hmm.
Bingo! Another allergy: Methylchloro- and methylisothiazolinone — preservatives found in, amongst other things, jet fuels and baby wipes.
A week later came my lab results. I was now diagnosed with CAU, chronic autoimmune urticaria (hives). Hesitant elation followed by new medications plus Xolair (allegedly an end-all-be-all treatment for CAU patients), a further culling of products, and a six-month wait-and-see period. Nada. I still had mind-numbing rashes, hives, and blistery evilness.
The Mayo Clinic, Scottsdale, Arizona: Year 10
At year 10, I was worse, but I had a team: A rheumatologist, a specialized gynecologist, an allergist, a dermatologist, and my primary care doctor. I was in doctors’ offices two-to-three times a week. Finally my team petitioned for me to go to the Mayo Clinic’s Scottsdale Campus. When I got the referral letter to see Dr. James Yiannias—I cried. If this guy couldn’t help me, no one could.
I had my Itchy File under my arm, an Evernote folder dedicated to years’ worth of rash-hivey photos, lists of failed medications and diagnoses, a request to test for autoimmune progesterone dermatitis, and a firm determination to understand the “why” behind The Itch.
I sat and talked with Dr. Yiannias for THREE HOURS. He never once checked his watch. He listened. He made notes. I told him that, through trial-and-error, I had discovered I was allergic not only to my diagnosed chemical allergens, but also to their siblings and kissing cousins. I told him that I had transfer issues, and that my husband had to use “my” products. I told him about the special kind of rosacea, the female hysteria, and my hives morphing into pimple-like papules. I told him about polymorphic light eruption and Black Oolong on my face. I told him about my symptoms spiking around my period. I told him about the European Standard Series test and its American cousin. I wasn’t leaving until I told him EVERYTHING I knew about My Itch and my journey to his office.
I told him I wanted a doctor-patient partnership, not a dictatorship. I told him I wanted my quality of life back. I told him I wanted a name for what ailed me. A cure. A way back to normal.
And he gave it to me. Two months after our initial sit-down, I endured my third chemical patch test. But this test was different. I was being tested with the Mayo Standard Series, the Mayo Cosmetic/Botanical/Fragrance Series, and the Mayo Hairdresser Series. I had 168 patches on my back—nearly five times the number of potential allergens as either of my previous tests. And, at my request he tested for autoimmune progesterone dermatitis. It was negative.
In the end, we discovered that I was allergic to 20 separate chemicals which have an astounding 1,896 mandatory cross-reactors (siblings) and 1,289 optional cross-reactors (cousins).

Me today.
After ten long, miserable, itchy, sleeping-with-icepack years, my tenacity led me to the correct diagnosis. The best part? Dr. Yiannias had previously developed a plug-and-play list of everyday products designed to eliminate product guesswork for people like me. That database is called SkinSAFE, and it is where I find products designed just for me.
Now I am the me that I used to be: Itch Free.
Read more in Your Ultimate Guide to Beautiful SkinBaseline series of patch test allergens. Dr. Amanda Oakley, Waikato Hospital, Hamilton New Zealand. DermNet NZ. Retrieved 18 September 2015.
http://www.dermnetnz.org/dermatitis/standard-patch.html.
Contact Dermatitis. Third Edition. 1986. Fisher, Alexander A.
Investigating the Causes of Chronic Itch: New Advances Could Bring Relief. National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIH). Retrieved 20 September 2015.
http://www.niams.nih.gov/News_and_Events/Spotlight_on_Research/2014/chronic_itch.asp.
Personal email communication. Yiannias, James A. Retrieved 15 September 2015.
SkinSAFE. http://www.skinsafeproducts.com/.





Add a Comment32 Comments
If anyone reading this has a surgical implant and cannot figure out what's going on with their body, look into that. I'm allergic to my breast implants and it's been a long journey of hearing that I'm insane from some doctors. Consultation is tomorrow!! :)
September 14, 2020 - 5:45pmThis Comment
Hi Anon
You make a great point - cosmetic breast implants (and others?) have caused with havoc with many women, and a leak can cause long term issues.
Please let us know how your consultation goes!
Best,
Susan
September 15, 2020 - 3:50pmThis Comment
Wow, what a story, I'm sorry for you but in the end all is good!!
September 4, 2020 - 7:24amThis Comment
Thank you for sharing your itchy story. I also have itchiness, but not to the extent you do. Thankfully, your persistence paid off. Now that we know your problem, we need to know how you are solving or learning to live with these allergies. Are you simply avoiding all allergens? How? Or is there a treatment?
August 2, 2020 - 6:12amThis Comment
Your story is very similar to mine, however I was lucky it only took 3 years and 5 dermatologist. All diagnosed contact dermatitis. But what products!? Finally a contact dermatitis specialist at Brigham & Women’s, the only specialist in Boston who could give me the test. MGH had a specialist leave. Called and got the earliest appt, 9 mths away! Thank goodness I asked to be put on a cancellation list! Two months later I got the 164 patch test, diagnosed & set me up with Skin Safe. A gift from God when the app was released. Better than the 40 page print out of approve items I was given when I walked out of her office. I get minor dry patches flare on my eyelids from time to time, but no where close to what it was. Swollen eyes almost shut. Fiery rash around my neck. It’s been 2 years of feeling comfortable in my skin again. Thanks for sharing your journey.
October 9, 2019 - 7:19pmThis Comment
The older I get, the more things make me break out in hives on contact. I've found that lavender oil, tea tree oil, & benedryl are the most effective itch stoppers.
Triggers sofar:
*Sizing, found in unwashed store clothing to stiffen product.
*Wool.
*A very particular tabby cat. No other cats or dogs do this.
*Scented laundry detergent & scented fabric softener.
*Dry-shaving with no lubricants.
*Perfume, cologne, insence, scented candles, but Fabreeze/Glade is okay.
*My car, which also triggers sneezing & difficulty breathing in the whole family.
*Grocery store convayor belts.
My mother has her own triggers:
January 23, 2019 - 2:00pm*The glue in some generic Breatherighs.
*Cosmetics.
This Comment
Amazing story! Good for you for not giving up and for the determination! It's your life and you deserve to live it fully, happily. I have sensitivities to make up, cosmetic products and don't know where to start.
April 12, 2018 - 8:24pmThis Comment
I’m curious to know what products you now are able to use?
January 21, 2018 - 7:25pmThis Comment
Shortly after giving birth I had 8 months of severe allergic symptoms very similar to what you have detailed. I visited 7 doctors, and had 6 rounds of allergy testing. In April I was diagnosed with allergies to 27 different contact allergens. It has definitely been an adjustment. I continue to flare up from products that are supposed to be safe, but it has gotten considerably better than prior to my diagnosis. I can't imagine dealing with that for 10 years. Thank you for sharing your story! It helps to hear there are others out there. I am going to ask about getting tested for the progesterone dermatitis. I have another autoimmune condition, and the dermatitis was most severe while I was breastfeeding (we breastfed to a year.) Have your symptoms gone away completely? Do you still run into allergens? Thanks!
August 3, 2017 - 7:50pmThis Comment
After working as an OR nurse for many years I developed a latex allergy which forced me to change my career. I have since developed allergies to perfumes, hypo allergenic medical tape, hair dye and bio oil. Boy I can relate to the ice pack story. When the itch is really really bad nothing will help apart from ice packs. The hair dye and bio oil reaction has occurred in the last month. I'm seriously considering shaving my head because my scalp is so irritated despite a course of steroids. Even my ears are weeping and blistered. Its reassuring it know that I'm not alone. I didn't think about transfer issues. I probably should see my specialist again to come up with a plan to sort out my current issues. Thank you for sharing your story.
July 18, 2017 - 1:27amThis Comment