When I was 32 years old in 2004, I had my future mapped out and was on the right track to achieve my goals. I was a mom of three young children, was happily married, and was in medical school training to become a respiratory therapist. What I didn’t know then as I read my medical textbooks was that I would soon end up with firsthand knowledge of life with a serious medical condition.
I first visited my doctor because I started having trouble swallowing and was experiencing more fatigue than even being a med student and mom of three could account for. The doctors told me I had thyroid cancer.
I went for a routine surgery to remove my thyroid and the cancer, called a thyroidectomy, and was home less than 24 hours later. But within 12 hours of being home my hands and feet were tingling and I felt very anxious, unable to sit still or rest. When I still wasn’t feeling better by that evening, my husband called the emergency room, and the doctors there said I should take some over-the-counter antacids to increase my calcium levels and come into the ER right away.
From the time we left the house to the time we arrived at the ER, my symptoms got even worse. My body was tingling from head to toe, and within minutes of arriving at the hospital I went into complete tetany (severe muscle cramping and spasms), which felt like having a severe Charlie horse everywhere at once. I was still awake and knew where I was, but my face had frozen completely, and my hands had tensed up to the point where my husband and the doctors couldn’t pry the washcloth I had been holding from my clawed grip. I knew I was in trouble because I had just enough medical training to know that they took me into the cardiac ER and I saw that they wheeled me past an elderly gentleman who had had a heart attack. I kept thinking how frightened my husband must be for me.
I was admitted to the hospital but I didn’t find out what had happened to me until the next day. At that point, the doctors told me that my parathyroid glands were not functioning, which they said was normal after thyroid surgery, and that my symptoms were the result of low calcium from not producing enough parathyroid hormone (PTH). They told me that I should take calcium along with vitamin D to help absorb the calcium and that my parathyroid glands would likely begin functioning again within six months. If they didn’t, the doctors said, the condition would be permanent and I would have something called hypoparathyroidism for the rest of my life.
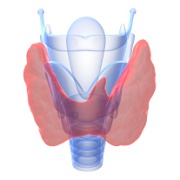
I learned that the parathyroid glands are four pea-sized glands located behind the thyroid that produce parathyroid hormone, which helps maintain appropriate levels of calcium and phosphorus in the blood. When the parathyroid glands are either damaged or removed, which can occur during thyroidectomy as in my case, the body may not produce enough—or any—PTH. (This can also occur as a result of certain autoimmune diseases or genetic conditions, or can occur without a clear cause.) Secreting low or no PTH is known as hypoparathyroidism, a condition that I learned affects only about 60,000 people in the U.S. and about 180,000 people worldwide. Before this, I had only ever briefly heard of the parathyroid glands. We had discussed them for about 15 minutes when we covered the endocrine system in my Anatomy and Physiology course.
I stayed in the hospital for nine days while doctors tried to regulate my calcium and phosphorus levels with pills and, eventually, through an IV. After I went home from the hospital, my life changed dramatically as I tried to keep my calcium levels balanced and learned to cope with my symptoms and the calcium and vitamin D regimen. The six months my doctor had mentioned in which things should have improved came and went, so I knew that the hypoparathyroidism was permanent. Before my surgery, I had been an active mom who loved to play outside with my family. After surgery, despite taking calcium and vitamin D, I continued to live with constant fatigue and bone pain, and tingling throughout my body that even today gets worse when I do too much activity. I became a spectator in my family’s life. I used to go out and do active things with them. Now they do active things while I watch. We go to Disney every year for Christmas, and now when we go I have to rent a scooter because I cannot walk very far without fatigue and pain. People glare at you and judge you when you are 42 and in a scooter—they think you’re lazy.
Over the past 10 years, I have also experienced some serious health concerns due to my use of the high doses of calcium required to manage my hypoparathyroidism symptoms. I learned that over time, long-term use of high doses of calcium and active vitamin D can cause hypercalcemia (high blood calcium) and vitamin D toxicity, leading to excess calcium in the urine, excess phosphate in the blood, and kidney damage. Patients also need the right amount of phosphorus, as too much can lead to kidney damage and calcium deposits throughout the body (soft tissue calcification). In my case, I have had several broken bones and fractures. I have broken one foot three times and the other twice, and also fractured my pelvis. I also suffered from kidney damage as a result of the high doses of calcium. The doctors have been able to reverse that damage, but now the fear is always in the back of my mind; when I have to take more calcium to manage my symptoms, I’m always wondering if that decision will lead to more kidney damage down the road.
As I learned to accept my new limits and lifestyle, I struggled with depression and guilt over not being able to do all the things I used to. With the support of my husband and my mother, I gradually became better at recognizing my own limits and knowing what would cause my symptoms to flare up, and learning not to feel guilty when I had to say no to certain activities. Now I have been able to finish school and go on to earn my Master’s and Doctorate degrees. Though being a practicing clinical respiratory therapist is not possible because of my hypoparathyroidism symptoms, I was able to turn my passion into an academic career, where teaching respiratory therapy to med students allows me to sit, stand, or rest as needed and gives me plenty of time to continue managing my condition.
It never dawned on me when I went for a one-day surgery that I would end up chronically ill forever.
All user-generated information on this site is the opinion of its author only and is not a substitute for medical advice or treatment for any medical conditions. Members and guests are responsible for their own posts and the potential consequences of those posts detailed in our Terms of Service.


Add a Comment2 Comments
Hi Christy, I have been postsurgical HPTH since 2010 and am so excited!!!! I am now on Natpara injections and feeling so much better. I reduced calcium from 2000mg daily to only 750mg and am completely off Rocaltrol. There is hope for us now!!!!!
September 15, 2015 - 12:36pmThis Comment
Hello ChristyM,
I would like to extend a very warm welcome to the EmpowHER community. Thank you for so bravely sharing your personal experience. It must have been very frightening for you and your family.
You have endured such physically suffering and emotional stress. Your story is inspirational. So glad that you were able to finish your education to such a high level and have found a way to use your knowledge and expertise to teach others.
Regards,
August 15, 2014 - 8:37amMaryann
This Comment