 Hemera/Thinkstock
Hemera/Thinkstock
In the United States, 94,293 people were on the waiting list as candidates for a kidney as of 11:55 am EST today, according to the Organ Procurement and Transplantation Network.
An individual would require a kidney transplant if she has kidney failure.
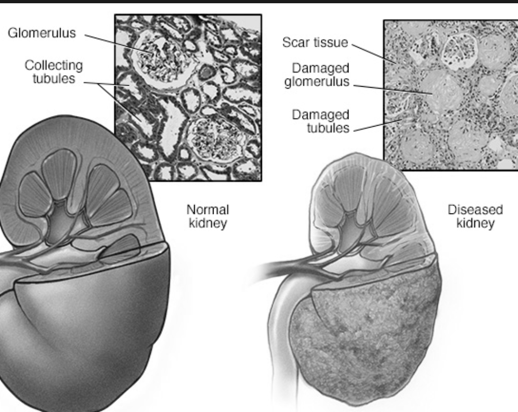
The most common causes in the United States of end-stage kidney disease, in which the kidneys can no longer function in the capacity needed, are high blood pressure and diabetes, according to MedlinePlus.
Patients in need of a kidney can wait several years for a donated organ. While waiting for a kidney, patients need to be on dialysis, a procedure which removes harmful substances from the blood — a function the kidney can no longer do.
Patients undergoing dialysis may need to have treatment three times a week, with each session lasting three to four hours.
To find a kidney suitable for the patient, the patient and kidney must be matched on certain factors: blood type and human leukocyte antigen, or HLA. A third factor, antibodies produced by the patient’s immune system, is also considered when finding a match.
If the patient’s immune system reacts to the donated organ, her body will not be able to accept this.
This is a significant issue for women and minorities waiting for kidney transplantation.
Jeffrey L. Veale, M.D., a UCLA transplant surgeon, explained that minorities, especially Hispanic and black individuals, have naturally higher antibodies. This can make it difficult to find a match for them, and they can sit on the deceased donor list for a long time, up to 10 years.
For women, the difficulty in finding a match may occur after having a baby.
Dr. Veale said that when a woman has a baby with her husband, she is exposed to her husband’s antibodies. If she needs a kidney later, her husband cannot be a donor, as her immune system has already made antibodies from her husband.
That is where living donors come in. Let’s say an individual wants to give a loved one a kidney, but she is not a match. Another person is a match for the loved one needing a kidney and donates that kidney.
Then the individual who was not a match for her loved one donates her kidney to someone else who is a match, starting a live donor chain. The chain keeps going because of altruistic donors, who do not expect to get anything back.
Dr. Veale noted that the altruistic donors are very special people. And because of them, people are able to get the kidneys they need. If an individual gets a kidney through a live donor chain, she is taken off the deceased donor list and someone else can move higher up on the list.
These living donor transplants are facilitated by the National Kidney Registry. Since the program started in February 2008, they have facilitated 563 transplants to date.
The largest U.S. multicenter study of living kidney transplant donor chains, of which Dr. Veale was senior study author, found that 46 percent of recipients were minorities and 50 percent were women. In comparison, of the living kidney transplants done in the U.S. in 2011, only 33 percent of recipients were minorities.
Live donor chains are life-changing for individuals waiting for a kidney. Keenan Cheung, a 47-year-old housing director at the University of Southern California, was born with a polycystic kidney. When he turned 40, his kidneys started to fail and he needed a transplant.
“I actually signed up for a kidney thru the normal UNOS lists via UCLA. As my wife and I started doing more research, we ran across the kidney exchange programs and how they increase your chances to get a kidney transplant faster. Additionally, research taught us that receiving a live donor kidney is better than a deceased donor kidney," Cheung said.
"Since I am O positive blood type, my chances to get a kidney through UNOS was not likely to happen quickly. We found [the] Johns Hopkins program and were in the process of signing up for their exchange. Around the same time, we received a letter from UCLA inviting us to join their exchange program. Since it was local, we signed up and joined their program.”
Having the kidney transplant facilitated through the live donor change significantly changed Cheung’s life.
“Quite frankly, I am happy I can pee. Both of my kidneys were not functioning and my CAPD was ineffective. I was going to change to hemodialysis if I didn’t receive the transplant when I did," Cheung said.
"My creatinine level was around 24 the month leading up to my transplant; my skin was dark, I was bloated, I couldn’t produce any urine for three months, I was tired and had no energy. During my transplant surgery, once the new kidney was hooked up, I produced 18 liters of urine. Can you imagine ... 18 liters of waste stored in one’s body?"
Cheung continued, "Three days after my surgery, I lost about 20 pounds of liquid, my creatinine was down to about 1.6, my skin tone had color ... amazing. I can swim, coach my kids, run and exercise. Other than the medicine I have to take daily, I have an amazingly active life ... My experience was so positive. If you saw me before and after, the change is unbelievable.”
Live donor chains help people find the kidneys they need, and often, the donors and recipients stay in touch. Dr. Veale stated that both parties must consent, but around 95 percent do. He said they look forward to meeting the people who saved their lives and stay in contact.
To learn more about live donor chains or to become a kidney donor, visit http://www.kidneyregistry.org/
References:
Interview with Jeffrey L. Veale, M.D. Phone. 23 October 2012.
Interview with Keenan Cheung. Email. 25 October 2012.
UCLA Newsroom. Nearly Half of Kidney Recipients in Living-Donor Transplant Chains are Minorities. Web. 31 October 2012.
http://newsroom.ucla.edu/portal/ucla/nearly-half-of-kidney-recipients-238975.aspx
Organ Procurement and Transplantation Network. Data. Web. 31 October 2012.
http://optn.transplant.hrsa.gov/data/
MedlinePlus Medical Encyclopedia. End-Stage Kidney Disease. Web. 31 October 2012.
http://www.nlm.nih.gov/medlineplus/ency/article/000500.htm
MedlinePlus Medical Encyclopedia. Dialysis. Web. 31 October 2012.
http://www.nlm.nih.gov/medlineplus/ency/article/007434.htm
National Kidney and Urologic Diseases Information Clearinghouse. Treatment Methods for Kidney Failure: Transplantation. Web. 31 October 2012.
http://www.kidney.niddk.nih.gov/kudiseases/pubs/transplant/
Reviewed October 31, 2012
by Michele Blacksberg RN
Edited by Jody Smith
keywords: kidney, kidney transplant, live donor chains, dialysis, immune system, antibodies, Dr. Veale, altruistic donors



Add a Comment3 Comments
Cristy....looks like some well thought out comments, but you can't have it both ways if there's "NO COMPREHENSIVE DATA" where is all your data coming from that you are quoting?
November 1, 2012 - 3:03pmThis Comment
This article is rife with falsehoods:
- 1/3 of folks on the kidney transplant wait list are 'inactive', meaning they couldn't have a transplant if a kidney became available.
- A transplant is a TREATMENT for end-stage renal disease, it is not a cure. Dialysis also a treatment for ESRD.
- Minority candidates have less access to transplants because A. they often lack access to healthcare, B. they are listed much later in their disease than their white counterparts, C. they more often lack insurance, D. a higher percentage have a rarer blood type (which has nothing to do with sensitivity), and E. they experience geographic disparities due to the uneven nature of the transplant system.
- According to a handout from the 2012 ASHI meeting, 30% of ALL transplant candidates are HLA sensitized. 15% of the wait list has had a prior transplant, the most common source of sensitization. Meanwhile, Women compose 40% of wait list candidates (OPTN data), and 80% of women aged 40-44 have children (US Census). This hardly translates into the article's inference that women who have children will be sensitized to their blood relatives' kidneys.
- ALL living organ donors are altruistic, not just the small portion that participates in a swap/pair or chain.
- No one receives a kidney through UNOS. OPTN is the membership organization under Dept of Health and Human Services which manages the transplant wait list. UNOS is simply the contractor.
And the biggie - a living donor kidney is 'better' than a deceased donor kidney.
Better for whom?
4.4 living kidney donors die in the US every year within 12 months of surgery.
20% experience complications: hernia, pancreatitis, chylous ascities, nerve damage, testicular swelling and sensitivity, etc.
20-30% suffer from depression, anxiety and/or PTSD. Not a single transplant center offers aftercare or support services.
We have NO NATIONAL STANDARDS of living donor care in the US. Every transplant center can make up it's own rules and is accountable to no one.
We have NO COMPREHENSIVE DATA on living donors' health and well-being. More than a decade after a federal mandate, we still have no idea if 35% of living donors are live or dead ONE YEAR after donation. After that, what happens to living donor is anyone's guess because no one bothers to track them.
Meanwhile, the Swiss LD registry reported 49% of their kidney donors with cardiovascular disease, 47% with hypertension and 45% with Stage 3/4 chronic kidney disease at only 10 years post-donation.
As the sister of a kidney transplant recipient, I understand the challenges of kidney disease. However, as a living kidney donor, I find the constant neglect of living donation's risks to the donor (not to mention poorly written articles such as this) to be unethical and dangerous. The public should never be viewed as medical supply. Living donors are people too.
www.livingdonor101.com
October 31, 2012 - 2:38pmThis Comment
How about the legals to become a donor if he/she from outside of US?
October 31, 2012 - 1:38pmAnd what is the procedures to take to become a donor in US if I'm a foreigner?
This Comment